As plans evaluate their pharmacy quality performance, it is important to consider what adjustments might be made to maintain the most effective outreach program to positively impact influence members’ medication use. This month, Luke Ellis, Manager of Client Operations at RxAnte, shares insight into how we develop the best medication adherence program for each health plan client.
Building a Successful Outreach Program
As Manager of Client Operations, I am responsible for overseeing health plan client implementations, intervention strategy, and evaluations to help improve the quality, cost, and member experience for the 14 million lives RxAnte manages. In working with various plans across the country, we find that regardless of the size or location of the plans’ contracts, there are four elements that remain key to building and executing a successful pharmacy quality outreach program:
- Effective Interventions
- Appropriate Targeting
- Appropriate Timing
- Intervention to Scale
Effective Interventions
Deploying effective intervention that can aid members in resolving barriers and influence member behavior is key to improving adherence in an MAPD population. To establish a strong foundation for any program, it is critical to consider the concept of balance. It would certainly create the most adherence impact if effective clinical callers were in regular contact with the majority of the membership. While health plans can—and often do—strive to conduct the most outreach possible, it is equally important to consider the potential risks of this approach in order to optimize program strategy based on available budget, internal resources, and program goals.
At RxAnte, we collaborate with plans to ensure they are deploying the most effective intervention mix possible for their unique population and in accordance with any business constraints. We achieve this while simultaneously considering the risks of member abrasion and effectively allocating intervention dollars. Starting in May, our clients eagerly await their Forecasts each month (portrayed below) to make real-time adjustments depending on performance. Plans trust our predicted Year-End results and our industry experience to know if any mid-year tweaks are required to maximize results.
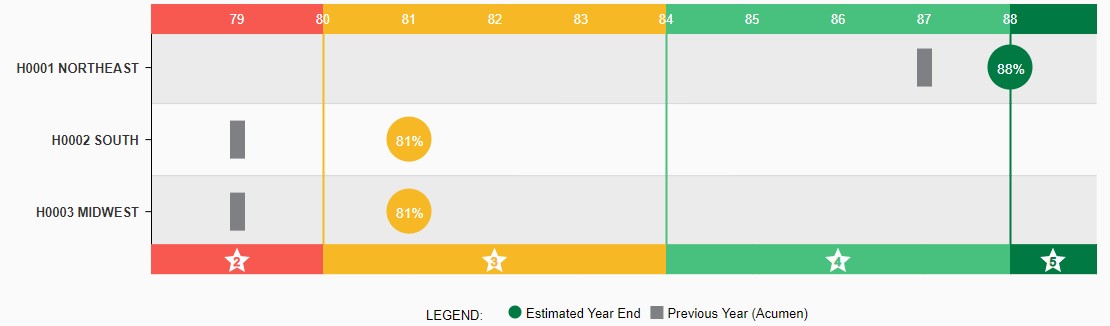
Accurate Targeting
Plans can adopt the approach of deploying the right mix of diverse intervention tactics, however if the right membership is not being targeted, these efforts may be misallocated and may not drive meaningful population-level adherence improvement to achieve a plan’s performance goals.
RxAnte’s risk stratification (visualized in the figure below) is a key component in deploying the right interventions to plan members that would benefit the most from a particular intervention. Our proprietary predictive analytics evaluate a plan’s population and place members into risk categories based on a number of factors, including member fill behavior and value of future adherence. We tailor a portfolio of recommended interventions to maximize a plan’s intervention budget and overall outreach effectiveness based on population mix and where membership falls in this risk stratification.
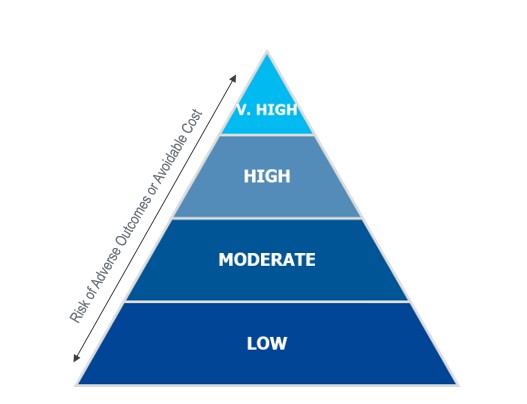
For example, those members who fall into the moderate-risk category can benefit from a more cost-effective method such as an automated reminder call or SMS text; in contrast, the highest-risk members may require more comprehensive, ongoing support like Mosaic Pharmacy Service, our high-value pharmacy solution. Mosaic is particularly suited for this highest-risk population—which, in certain instances, can represent over 50 percent of non-adherent members and nearly 20 percent of all medical and pharmacy costs1—due to the service’s focus on resolving longstanding adherence barriers including regimen safety, complexity, and cost for medically complex members.
Appropriate Timing
Next in the foundational elements is timing. Specifically, interventions must target the right member at the right time in order to generate the maximum impact on overall quality improvement. Many health plans are deploying interventions based on lists that are refreshed only once a month; this is far too infrequent to ensure the necessary members are receiving the appropriate intervention to meaningfully improve medication use.
At RxAnte, a key benefit in our approach is the ability to provide our clients with prioritized lists on a weekly basis to create a streamlined, efficient outreach process. Additionally, we offer the industry’s only adherence workflow solution tool, RxEffect, to further improve member engagement and simplify the outreach experience for internal pharmacy quality teams. We built this unique solution on a patented analytics platform that updates prioritized outreach lists every day to ensure plans are acting on timely and accurate data.
Intervention to Scale
The last piece to incorporate is how to reach enough high-priority people to achieve meaningful improvement in quality measures. It is imperative for plans to scale their outreach volume appropriately to influence enough members to impact population-level adherence rates.
At RxAnte, we consider individual staffing and budgeting constraints and utilize our predictive simulations to help plans make a capacity strategy that is right for them. Through ongoing collaboration, reporting, and evaluation of a plan’s program, we aim to find that optimal subset of members that is large enough to positively influence plan’s quality metrics and small enough to diminish the risks of member abrasion and reduced member satisfaction.
By coupling these four pillars to develop an intelligent and strategic outreach program, our clients continue to see year-over-year improvement in their pharmacy quality scores. Want to learn how we can help improve your Star Ratings and member medication use? Contact us today for a free, no-obligation evaluation of your population.
REFERENCES:
1 RxAnte analysis of client health plan data